MDaudit recently hosted a webinar titled, Revenue Integrity in 2026: Predictions, Priorities, and Payer Reality. The session brought together benchmarking data, frontline trends, and a clear message for healthcare leaders: revenue integrity is a critical revenue cycle strategy.
Drawing on insights from more than $20B in annual charges audited, $200B+ in denials analyzed, and 1.5M+ cases reviewed each year, the discussion focused on one theme: how the revenue cycle is redefining revenue integrity.
Revenue Integrity Is Now a Cross-Functional Revenue Cycle Discipline
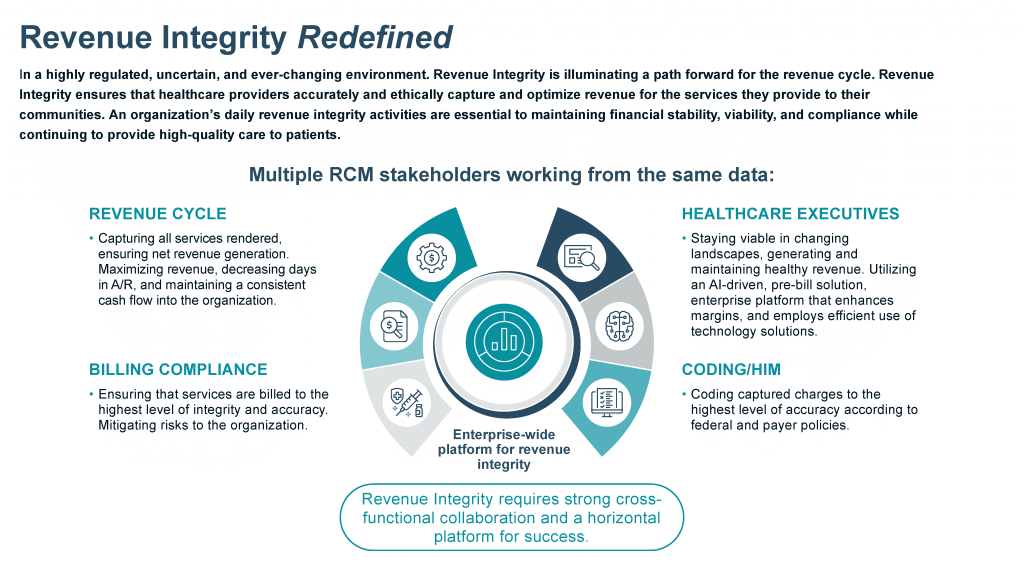
Revenue integrity has traditionally been associated with compliance and post-bill audits. That model no longer holds up.
Today, revenue integrity sits at the center of:
- Billing and payments data
- Coding accuracy and governance
- Clinical documentation and system edits
- Denial management
- Patient financial experience
Different stakeholders ask different questions from the same dataset. Billing operations want to know if claims are clean and timely. Coding leaders focus on accuracy and regulatory updates. Clinical and IT teams evaluate documentation and edit logic. Executives look at lag days, denial dollars, and audit exposure.
The takeaway from the webinar was clear: revenue integrity connects these functions. When it operates in silos, risk multiplies. When it operates as a coordinated revenue cycle discipline, financial performance stabilizes and even excels.
Webinar highlights:
- Denials Are Rising Across Every Setting
One of the most urgent themes discussed was denial growth.
In 2025:
- Average denied amounts increased 14% in hospital outpatient settings
- Denied amounts increased 12% in inpatient settings
- Coding-related denials in outpatient care rose 26%, building on a 126% increase the prior year
Errors in diagnosis coding, modifier usage, and insufficient documentation were the primary drivers.
Outpatient coding accuracy has become a defining financial lever. As more care shifts to outpatient settings, small coding variances scale quickly. When organizations deploy automation without governance, risk compounds. The message was not to slow down technology adoption, but to wrap it in oversight.
Revenue integrity teams that add a closed-loop coding integrity layer are better positioned to reduce rework, avoid preventable denials, and protect reimbursement.
- Medicare Advantage and RFI Denials Are Escalating
The webinar also examined trends tied to Medicare Advantage and RFI or medical necessity denials.
In 2025:
- The average denied amount for Medicare Advantage increased 20%
- RFI and medical necessity denial dollars tied to Medicare Advantage increased nearly fivefold, from $161 to $789 per claim
- Across all care settings, average denied amounts tied to RFI and medical necessity rose sharply
These shifts reflect tighter payer scrutiny and increased pre-authorization and documentation demands. Providers are absorbing longer review timelines and higher financial exposure per case.
This environment reinforces the need for proactive revenue cycle monitoring. Waiting until the denial hits the AR report is too late. Revenue integrity must influence pre-bill review, documentation workflows, and payer contract discussions.
- Commercial Payers Are Slowing Initial Claim Responses
Another major insight centered on lag days.
In 2025, commercial payers increased the time required to adjudicate initial claims:
- +3 days for inpatient hospital claims
- +7 days for outpatient hospital claims
- +9 days for professional claims
On average, hospital claims exceeded 30 days for initial response. Professional claims approached five weeks.
Lag days function as a leading indicator. When adjudication timelines stretch, working capital tightens. Across millions of encounters, even a few additional days can create significant cash flow strain.
Health systems that track average lag days and tie them back to upstream billing and coding performance are better positioned to identify breakdowns and hold payers accountable.
- Payer Audits and At-Risk Revenue Are Growing
External payer audit activity increased substantially in 2025.
- Total at-risk amounts per customer increased 30%
- Audit cases per customer also increased 30%
- The average at-risk amount per hospital audit approached $17,000
Commercial payers drove 45% of at-risk amounts. Medicare and Medicaid accounted for 28%.
Coding errors, medical necessity challenges, billing errors, and missing information were among the top drivers of audit requests. Diagnosis-Related Group coding, procedure coding, and investigational device usage surfaced as recurring themes in hospital settings.
The operational impact is significant. Without centralized audit tracking and risk monitoring, organizations struggle to respond efficiently. The webinar emphasized that continuous monitoring tools can reduce audit response times and create tighter oversight of at-risk revenue.
- Auto-Downcoding and Compliance Exposure
The session also addressed a growing concern: automatic downcoding by Medicare Advantage plans.
Hospitals are increasingly receiving reduced payments based on payer reclassification of level of care or service intensity. Accepting these payments without formal appeal review can introduce compliance exposure, including potential False Claims Act implications.
Revenue integrity teams must evaluate not only whether they can recover dollars, but whether they are managing regulatory risk appropriately. This is another example of how the revenue cycle now intersects directly with compliance governance.
2026 Predictions: Prevention, Monitoring, and Intelligent Workflows
Looking ahead, the webinar outlined four clear predictions for 2026.
1. Denials Will Become More Complex and More Preventable
Organizations that shift focus to pre-bill review supported by predictive analytics and structured workflows will reduce preventable denial volume.
2. Payer Audits Will Escalate
Continuous risk monitoring and centralized audit management will shorten response times and limit exposure.
3. Technology Adoption Will Drive Operational Stability
AI-powered revenue integrity platforms are expected to improve operational efficiency and denial overturn rates, particularly when paired with governance controls.
4. Outpatient Coding Accuracy Will Define Financial Performance
As outpatient volume grows, coding precision becomes central to margin protection.
Revenue Integrity Is the Revenue Cycle’s Control Center
The most consistent theme throughout the webinar was that revenue integrity now functions as the control center of the revenue cycle.
It connects:
- Upstream documentation and coding
- Mid-cycle claim submission and edit logic
- Downstream denial and audit management
- Executive financial oversight
Organizations that treat revenue integrity as an isolated audit function will continue reacting to denials and payer audits. Those that embed revenue integrity across the revenue cycle will identify risk earlier, correct it faster, and create measurable financial stability.
For healthcare leaders evaluating their 2026 priorities, the message is straightforward: revenue integrity is an operating model. Want to learn more?
Catch the on-demand recording of this webinar or contact us.



